Our Priorities
Let’s make healthcare equitable for all
With your support, MAP Centre for Urban Health Solutions will break down barriers to healthcare.
Let’s create the trauma centre of the future
Your gift will help Canada’s top trauma hospital provide wraparound care for trauma patients in one healing space.
Let’s stop multiple sclerosis in its tracks
With your support, the BARLO MS Centre will deliver the holistic care that people with MS deserve and discover how to stop the disease, once and for all.
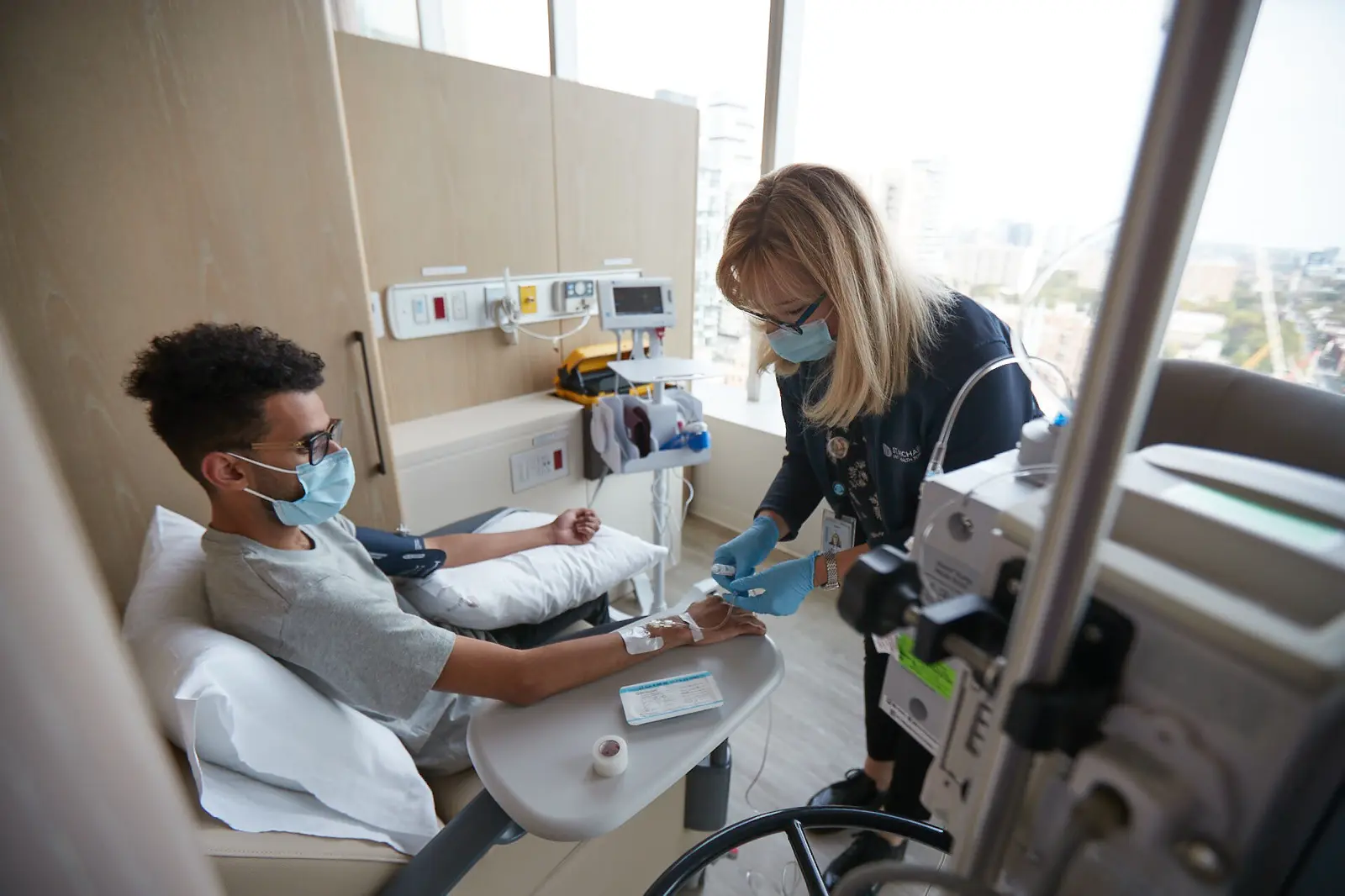
Let’s revolutionize brain and heart care
Your donation will help The Schroeder BRAIN&HEART Centre discover new ways to treat brain, heart and vascular diseases.
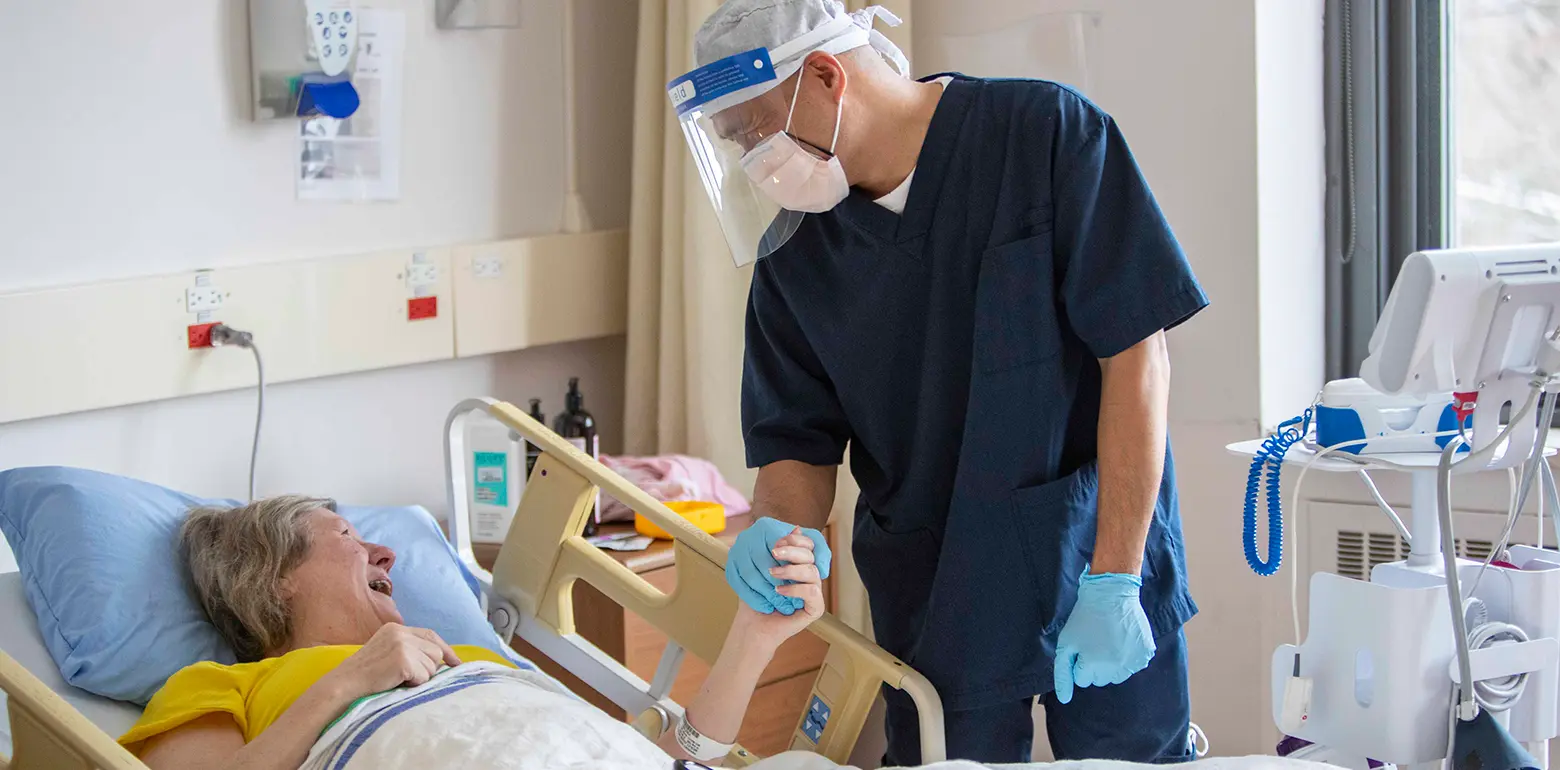
Let's take critical care to the next level
With your support, Canada’s premier critical care hospital will be a global leader in the art and science of critical care.
Join Us

Thank Your Healthcare Champions
Show your appreciation by donating in support of St. Michael's Hospital.
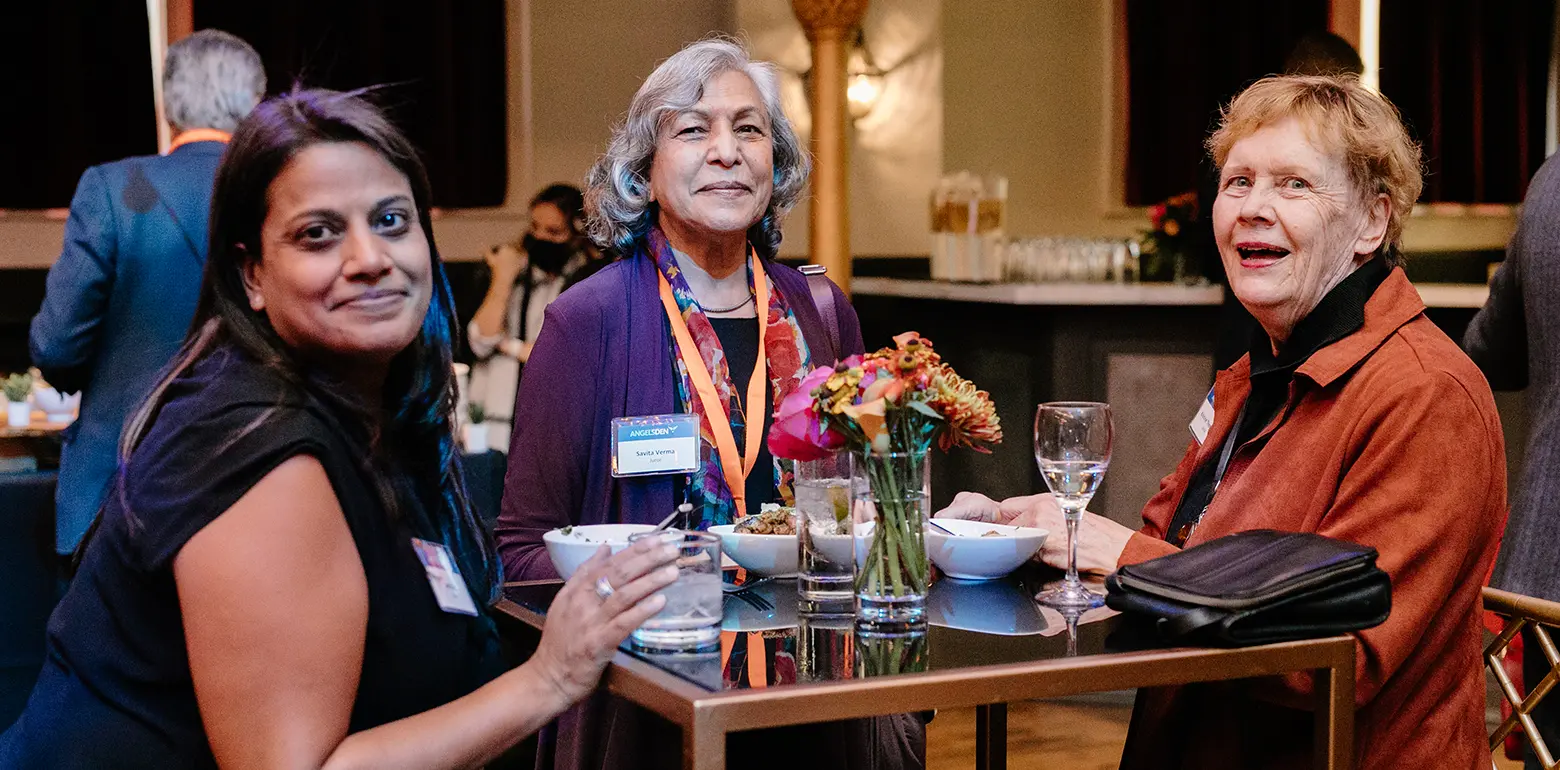
Attend Our Events
Join us and see first-hand how our world-leading experts are reinventing the patient experience.

Start a Fundraiser
Get creative and fundraise your way to helping us deliver the care our patients deserve.

Donate
Your generosity empowers our health teams to advance excellence, spark innovation, and champion equity.
Get in Touch
Have a question? Want to learn more about the Foundation’s work and how you can get involved? We’d love to talk with you.
| Telephone: 416 864 5000 | Email: hello@stmichaelsfoundation.com |